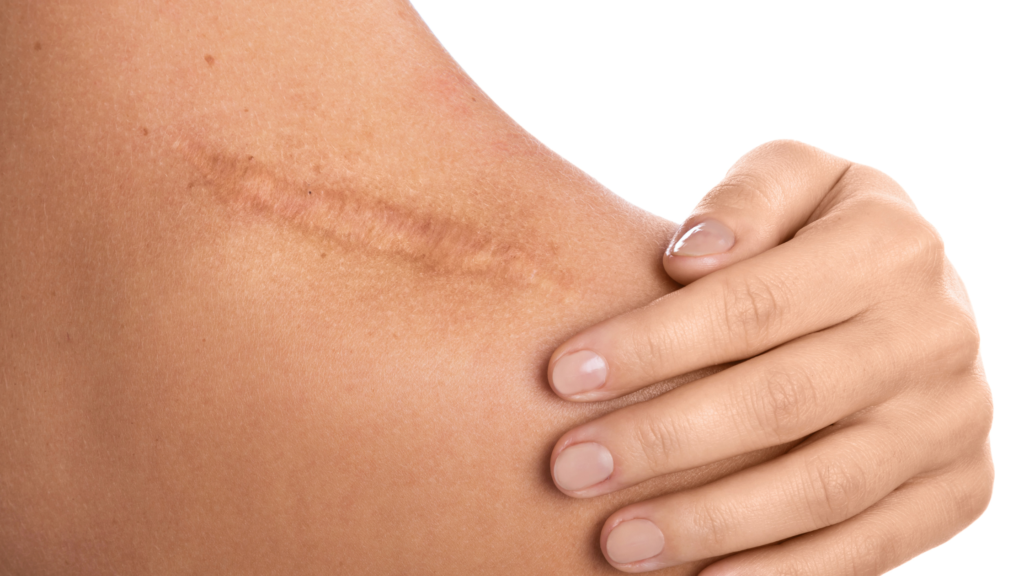
Yes, keloids are significantly more common in darker skin types, with Black African and Afro-Caribbean populations showing 15-20 times higher prevalence than white Europeans.
This dramatic difference reflects biological factors rather than environmental or healthcare access issues. Understanding why darker skin types develop keloids more frequently helps high-risk individuals take preventive measures and seek appropriate treatment.
Keloid Prevalence by Skin Type in UK
Ethnicity represents the strongest predictor of keloid risk. UK demographic diversity provides clear evidence of these differences.
Black African and Afro-Caribbean Populations
Prevalence reaches 15-20% in Black African and Afro-Caribbean communities, making keloids extremely common. This compares to 0.09-1% in white European populations, representing a 15-20 fold difference. In London’s diverse population, keloid clinics see predominantly Black patients despite this group comprising only 13% of the city’s population.
South Asian Communities
Indian, Pakistani, and Bangladeshi populations show intermediate keloid rates at 5-10% prevalence. This represents 5-10 times higher risk than white Europeans but lower than Black populations. UK South Asian communities, comprising approximately 9% of the population, account for disproportionate keloid cases in dermatology services.
East Asian Populations
Chinese, Japanese, and Korean individuals demonstrate keloid rates of 3-7%, falling between South Asian and white European prevalence. Whilst lower than other minority groups, East Asians still show 3-7 times elevated risk compared to white populations. UK East Asian communities report keloid concerns frequently enough to warrant culturally appropriate treatment approaches.
Fitzpatrick Skin Type Classification
Dermatologists use the Fitzpatrick scale to classify skin types and predict keloid risk. Understanding your Fitzpatrick type helps assess personal risk.
| Fitzpatrick Type | Description | Keloid Risk | Ethnic Groups |
| I-II | Very fair, burns easily | Very Low (0.09-0.5%) | Northern European |
| III | Fair to medium | Low (0.5-1%) | Southern European |
| IV | Olive to light brown | Moderate (3-5%) | Mediterranean, East Asian |
| V | Brown | High (8-12%) | South Asian, Hispanic |
| VI | Dark brown to black | Very High (15-20%) | Black African, Afro-Caribbean |
Types I-III (Fair Skin)
White European populations predominantly fall into Types I-III, showing minimal keloid susceptibility. When keloids develop in fair-skinned individuals, they typically follow significant trauma like burns or major surgery. Spontaneous keloid development from minor injuries remains rare.
Types IV-V (Medium to Brown Skin)
Mediterranean, South Asian, and East Asian populations typically classify as Types IV-V. These groups show moderate to high keloid risk, particularly following acne, surgery, or ear piercing. Family history becomes particularly relevant for predicting individual risk within these populations.
Type VI (Dark Brown to Black Skin)
Black African and Afro-Caribbean individuals predominantly classify as Type VI, showing highest keloid susceptibility. Even minor trauma like ear piercing or small cuts can trigger keloid formation. This extreme sensitivity makes prevention strategies crucial for Type VI individuals.
Biological Mechanisms Behind Increased Risk
Fibroblasts from darker-skinned individuals demonstrate increased collagen production and prolonged cellular activity during wound healing. Multiple genes associated with keloid susceptibility show higher frequency in African and Asian populations, affecting TGF-β signalling and collagen regulation.
Enhanced inflammatory responses in darker skin, whilst aiding infection prevention, also increase excessive scar formation risk through sustained collagen production signals.
UK Demographics and Keloid Burden
London’s diverse population includes approximately 13% Black and 20% Asian residents, creating substantial keloid patient populations.
Urban specialist keloid services see patient demographics reflecting these elevated risk groups disproportionately. Rural areas with predominantly white populations report lower overall prevalence, though minority populations show identical ethnic-specific rates.
NHS keloid treatment availability often fails to match demand in multicultural urban centres.
Common Triggers in Darker Skin Types
Ear piercing proves particularly problematic for Type V-VI individuals, with 10-15% of Black individuals developing ear keloids post-piercing. Cartilage piercings carry especially high risk at 20-25%. Chest and back acne frequently progresses to keloids in darker skin, making early acne treatment crucial. BCG vaccination scars cause keloids in approximately 5% of Type VI individuals.
Treatment Considerations for Darker Skin
Keloid treatment in darker skin types requires specific considerations. Certain therapies carry different risks depending on skin phototype.
Laser Therapy Cautions
Laser treatments for keloids risk post-inflammatory hyperpigmentation (PIH) in darker skin. Nd:YAG lasers prove safer for Type IV-VI skin than other laser types, but still require careful parameter adjustment. Advanced laser protocols must account for melanin content to avoid pigmentation complications.
Steroid Injection Effects
Intralesional steroids work effectively across all skin types but may cause hypopigmentation (lightening) in darker skin. This creates visible colour mismatch between treated keloid and surrounding skin. Patients should understand this trade-off when considering steroid treatment, though most prefer flat, lighter scars over raised keloids.
Surgical Considerations
Surgical excision carries identical recurrence risks across skin types but wound healing differences matter. Darker skin shows more robust scarring responses, making comprehensive post-operative protocols particularly crucial. Specialist surgical revision with appropriate aftercare proves essential for Type V-VI patients.
Prevention Strategies for High-Risk Individuals
Type V-VI individuals should carefully consider elective ear piercing, tattoos, or cosmetic procedures. Pressure earrings post-piercing or prophylactic steroid injections at surgical sites may reduce risk. Any scar showing abnormal characteristics requires immediate assessment. Recognising early signs and early treatment prevents progression to large lesions.
Cultural and Social Considerations
Visible keloids cause significant psychological distress across all ethnicities, but minority populations may experience compounded stress affecting professional opportunities. Some cultures view keloid scarring differently, whilst others find it particularly disfiguring.
Minority communities may face barriers accessing specialist care including language difficulties or financial constraints. Private specialist services work to provide culturally sensitive care whilst delivering appropriate medical intervention.
UK diversity enables comparative studies examining genetic versus environmental factors, with London hospitals providing comprehensive data on keloid prevalence across ethnic groups. NHS data reveals minority populations delay treatment longer, often presenting with larger keloids. Understanding these patterns helps improve early intervention programmes.
Treatment Outcomes and Genetic Considerations
All skin types respond to intralesional steroids (60-80% improvement), though darker skin may show hypopigmentation. Surgical recurrence rates show minimal difference by ethnicity when comprehensive aftercare follows. Proper treatment protocols prove more important than ethnicity for long-term success.
Keloid susceptibility involves multiple genes, making inheritance complex. Children of keloid-prone parents carry elevated risk but not certainty. Severity doesn’t predict offspring outcomes, making precise counselling difficult. Most children of keloid-prone parents avoid significant problems.
Conclusion
Keloids are dramatically more common in darker skin types, with Black African and Afro-Caribbean individuals showing 15-20 times higher prevalence than white Europeans. This difference reflects genetic and biological factors affecting wound healing and collagen regulation. High-risk individuals in the UK should take preventive measures and seek early specialist treatment when keloids develop.
Frequently Asked Questions
Why are keloids more common in Black skin?
Genetic factors affecting fibroblast activity, collagen production, and inflammatory responses show higher frequency in African ancestry populations. These genes create heightened scarring responses that produce keloids more readily. The difference is biological rather than environmental, which explains consistent patterns across geographic locations including the UK.
Do all Black people get keloids?
No, only 15-20% of Black individuals develop keloids despite the elevated risk compared to other ethnic groups. Having genetic susceptibility doesn’t guarantee keloid formation; triggering injury is also required. Many Black individuals never develop keloids despite ancestral predisposition.
Can white people get keloids?
Yes, though much less commonly at 0.09-1% prevalence. White individuals who develop keloids typically experience them following major trauma like burns or extensive surgery. Spontaneous keloid development from minor injuries remains extremely rare in white populations.
Are keloid treatments different for darker skin?
Treatment principles remain similar across skin types, but darker skin requires specific precautions. Laser therapy needs parameter adjustments to avoid pigmentation issues. Steroid injections may cause visible hypopigmentation in darker skin. Specialist expertise with darker skin types optimizes outcomes.
Should I avoid ear piercing if I’m Black?
Personal risk assessment matters more than blanket recommendations. If you have a family history of keloids or previous abnormal scarring, ear piercing carries substantial risk. Many Black individuals pierce ears without problems, but approximately 10-15% develop keloid complications.
Do keloids look different on darker skin?
Keloids show similar physical characteristics across skin types (raised, firm, extending beyond injury). However, colour differences prove more pronounced in darker skin where keloids often appear significantly darker than surrounding skin. This colour contrast makes keloids particularly noticeable on Type V-VI skin.
Are research and treatments improving for darker skin keloids?
Yes, increasing recognition of health disparities drives keloid research in diverse populations. Understanding genetic mechanisms specific to African and Asian ancestry populations improves targeted treatments. UK diversity provides opportunities for world-leading research addressing keloid burden in high-risk communities.