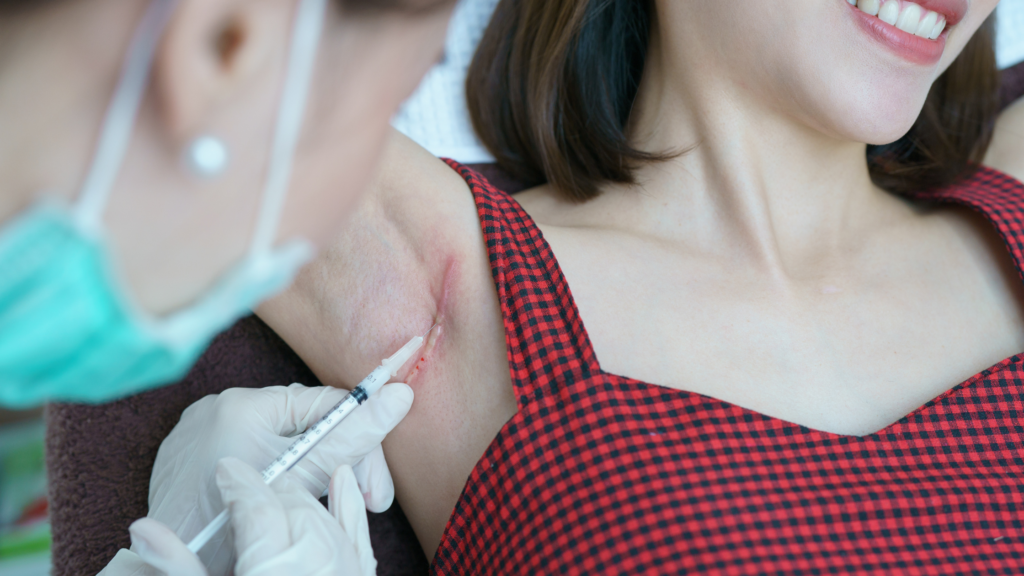
The NHS does offer keloid treatment, but availability varies dramatically between regions and clinical commissioning groups. Many patients discover that NHS keloid services are limited to symptomatic cases, with long waiting times and restricted treatment options.
Understanding what the NHS can and cannot provide helps you make informed decisions about your keloid care.
NHS Keloid Treatment Availability Across the UK
NHS keloid treatment exists but operates under strict eligibility criteria and resource constraints. Access depends heavily on your location, keloid characteristics, and local commissioning decisions.
Regional Variation in Services
NHS keloid services differ substantially between England, Scotland, Wales, and Northern Ireland. Some clinical commissioning groups (CCGs) provide comprehensive keloid treatment whilst others offer only basic steroid injections.
London typically offers better access due to teaching hospitals and specialist dermatology units, whilst rural areas may have no local keloid services.
Referral Pathways and Waiting Times
GP referral to dermatology or plastic surgery represents the standard pathway for NHS keloid treatment. Waiting times for initial consultation typically range from 3-12 months depending on region and service demand. Treatment itself then requires additional waiting, meaning total time from GP referral to receiving treatment often exceeds 12-18 months.
What Treatments the NHS Typically Offers
NHS keloid treatment usually focuses on steroid injections (triamcinolone) as first-line therapy. Some centres offer cryotherapy, surgical excision, or laser treatment, but these remain less widely available. Advanced therapies like combination protocols, pressure therapy, or newer technologies are rarely accessible through NHS services.
NHS Eligibility Criteria for Keloid Treatment
The NHS prioritises keloid cases based on medical need rather than cosmetic concerns. Understanding eligibility helps set realistic expectations about NHS access.
Symptomatic vs Cosmetic Classification
NHS treatment typically requires keloids to cause physical symptoms such as pain, itching, or functional impairment. Purely cosmetic concerns, where the keloid causes psychological distress but no physical symptoms, often don’t meet funding criteria. This distinction proves frustrating for patients whose keloids significantly impact quality of life despite being “asymptomatic” in medical terms.
Location and Size Considerations
Keloids affecting functional areas like joints or causing movement restriction receive priority. Facial keloids occasionally qualify due to psychological impact being considered clinically significant. Large or rapidly growing keloids typically receive faster referral than small, stable scars.
Previous Treatment History
Patients who have tried over-the-counter treatments without success may strengthen their case for NHS referral. Previous private treatment that failed doesn’t necessarily help NHS applications, as CCGs may question why further NHS resources should be allocated. Documentation of symptoms, functional impact, and failed conservative measures supports referral requests.
What NHS Keloid Treatment Actually Includes
When NHS treatment is approved, the scope often differs from comprehensive private care. Understanding what’s typically provided helps manage expectations.
| Treatment Type | NHS Availability | Typical Limitations |
| Steroid Injections | Widely available | Limited to 2-4 sessions, basic technique |
| Cryotherapy | Some centres only | Older equipment, fewer sessions |
| Surgical Excision | Selected cases | Limited post-op care, basic techniques |
| Laser Therapy | Rare | Teaching hospitals only, long waits |
| Pressure Therapy | Very limited | Minimal support/monitoring |
| 5-FU Injections | Uncommon | Specialist centres only |
Steroid Injection Protocols
NHS steroid injections typically use basic triamcinolone without advanced delivery systems or pain management technology. Sessions are often limited to 2-4 treatments regardless of keloid response. Follow-up appointments may be infrequent, and maintenance therapy to prevent recurrence is rarely offered systematically.
Surgical Options
NHS surgical excision is generally reserved for large, symptomatic keloids causing significant functional problems. Post-operative care may be less comprehensive than private protocols, potentially increasing recurrence risk. Reconstructive techniques for ear keloids or complex cases may not be available at all centres.
Advanced Therapies
Laser treatment, cryotherapy, and combination protocols remain uncommon in NHS settings. Where available, these typically exist only at teaching hospitals or specialist centres with substantial waiting lists. Newer technologies like radiofrequency or advanced LED therapy are almost never accessible through NHS services.
NHS Waiting Times for Keloid Treatment
Time delays represent one of the biggest challenges with NHS keloid care. Understanding typical timelines helps patients decide whether to pursue private treatment.
Initial Consultation Wait
From GP referral to first dermatology or plastic surgery appointment typically takes 3-6 months in well-resourced areas. In areas with fewer specialists or higher demand, waits can extend to 12 months or more. Urgent cases may receive faster appointments, but keloids rarely qualify as urgent unless causing severe symptoms.
Treatment Commencement
After initial consultation, starting treatment requires additional waiting for appointment scheduling and treatment room availability. This typically adds 2-4 months to the timeline. For surgical cases, waiting lists can extend 6-12 months from decision to operate.
Total Time to Treatment
Realistically, patients should expect 6-18 months from initial GP visit to receiving actual keloid treatment through the NHS. For complex cases requiring multiple treatments or surgical intervention, the complete treatment course may span 2-3 years including follow-up.
Limitations of NHS Keloid Services
Beyond access and waiting times, NHS keloid treatment faces inherent limitations affecting outcomes. These constraints reflect resource pressures rather than clinical expertise.
Limited Treatment Sessions
Budget constraints often limit steroid injection courses to 2-4 sessions regardless of clinical response. Private protocols typically provide 6-8 initial sessions plus maintenance, which research shows produces better outcomes. Stopping treatment prematurely due to session limits frequently results in partial improvement followed by recurrence.
Basic Equipment and Technology
NHS services typically use standard equipment without advanced features like automated cooling or precision delivery systems. Whilst clinically effective, basic equipment may cause more discomfort and less consistent results. Newer technologies that could improve outcomes often aren’t available due to procurement constraints.
Inconsistent Follow-Up
Post-treatment monitoring may be minimal or inconsistent in NHS settings. Patients might receive 2-3 follow-up appointments then be discharged regardless of keloid behaviour. This limited surveillance means recurrence signs may not be caught early when intervention is most effective.
Misdiagnosis and Inappropriate Referral Pathways in NHS Keloid Care
One of the most significant yet under-recognised challenges within NHS keloid treatment pathways is initial misdiagnosis or misclassification of keloid scars, which can lead to inappropriate referrals and suboptimal outcomes.
Keloids are not simply “lumps” — they are a distinct form of pathological scar with a well-understood biological behaviour. However, when the initial assessing clinician is unfamiliar with keloid pathology, these lesions may be incorrectly treated as non-specific soft tissue masses. This often results in referral based on anatomical location rather than underlying pathology.
A common example is keloid formation in the pubic or groin region, frequently arising from:
- Poor hair removal practices
- Recurrent ingrown hairs
- Chronic folliculitis
In such cases, patients are often referred to gynaecology services rather than dermatology or specialist scar clinics. Due to limited familiarity with keloid disease in these settings, lesions may be:
- Surgically excised as isolated lumps
- Managed without appropriate diagnosis of keloid biology
- Discharged without structured follow-up
This approach is problematic. Simple excision of a keloid without adjunctive therapy carries a very high recurrence rate, often resulting in:
- Rapid regrowth
- Larger and more irregular scar formation
- Increased symptoms (pain, itching, inflammation)
- Significant psychological distress
At Rejuvence Clinic, we frequently see patients who have undergone such pathways. Many present with recurrent keloids that are larger, more complex, and more difficult to treat than the original lesion. In these cases, management often requires:
- Revision surgery under specialist protocols
- Intralesional steroid therapy
- Laser or adjunctive treatments
- Long-term follow-up and recurrence prevention strategies
Ultimately, even with the best intentions, lack of familiarity with keloid disease can lead to well-meaning but counterproductive interventions. Incorrect referral pathways and overzealous surgical management without preventative measures can significantly worsen outcomes and delay effective treatment.
This highlights the importance of:
- Early recognition of keloid pathology
- Referral to appropriate specialists (dermatology or keloid-focused services)
- Use of combination treatment protocols rather than surgery alone
Without this, patients may experience a cycle of recurrence and escalation — often leading them to seek private specialist care after avoidable deterioration in their condition
Comparing NHS and Private Keloid Treatment
Understanding the differences between NHS and private care helps patients make informed choices about their treatment pathway. Both systems have experienced clinicians, but service models differ substantially.
Treatment Comprehensiveness
Private clinics like Rejuvence Clinic offer comprehensive protocols combining multiple treatment modalities tailored to individual cases. NHS services typically provide single-modality treatmentwith limited combination approaches. This difference significantly affects outcomes, particularly for resistant or recurrent keloids.
Technology and Innovation
Private clinics invest in advanced technologies like TargetCool pain management, automated cryotherapy, and modern laser systems. NHS services use proven but basic equipment that, whilst effective, may not provide the same comfort or precision. Access to newer treatment options happens years earlier in private settings.
Continuity and Personalisation
Private treatment typically involves consistent practitioner relationships and personalised protocols adjusted based on response. NHS treatment may involve different clinicians at each visit with less individualised adjustment. This continuity affects treatment optimisation and patient confidence.
Cost Considerations: NHS Free vs Private Investment
Whilst NHS treatment is free at point of use, hidden costs and treatment limitations create trade-offs. Private treatment involves upfront costs but may prove more cost-effective long-term.
True Cost of NHS Treatment
NHS keloid treatment carries no direct financial cost to patients, which represents significant value. However, indirect costs include time off work for multiple appointments, travel expenses, and potential lost earnings during extended waiting periods. Failed NHS treatment requiring subsequent private care means patients ultimately pay whilst losing time.
Private Treatment Investment
Private keloid treatment costs in London range from £115 for basic steroid injections to several thousand pounds for comprehensive surgical revision.
Whilst representing substantial investment, faster access, better technology, and comprehensive protocols often produce superior outcomes.
Many patients find private treatment cost-effective compared to years of NHS waiting and potentially incomplete treatment.
Value Proposition Analysis
For patients with symptomatic keloids affecting quality of life, private treatment’s faster timeline and comprehensive approach may justify the investment. For small, stable keloids causing minimal impact, NHS treatment remains appropriate if patients can tolerate waiting times. Those with higher keloid risk based on ethnicity or family history may benefit from earlier private intervention preventing progression.
When NHS Treatment May Be Sufficient
Despite limitations, NHS keloid services appropriately serve certain patient groups. Understanding when NHS treatment meets needs prevents unnecessary private expenditure.
Small, Early-Stage Keloids
New, small keloids responding well to initial steroid injections may achieve good outcomes through NHS treatment. If the keloid shows significant flattening after 2-3 NHS sessions, the service level may prove adequate. Patients can always pursue private treatment later if the NHS approach proves insufficient.
Keloids in Low-Risk Locations
Keloids on less visible areas like the upper back or shoulders causing minimal functional impact may not require advanced private treatment. If the primary concern is reducing symptoms rather than achieving optimal cosmetic results,
NHS services may suffice. Patients prioritising symptom control over appearance often find NHS treatment acceptable.
Patients with Time Flexibility
Those able to wait 12-18 months for treatment without significant distress may reasonably pursue NHS options first. If keloids are stable rather than rapidly growing, delayed treatment poses less risk. Patients should monitor keloids during waiting periods and switch to private care if rapid growth occurs.
When Private Treatment Becomes Necessary
Certain keloid presentations require advanced intervention beyond typical NHS capabilities. Recognising these situations helps patients avoid wasting time on inadequate treatment.
Recurrent Keloids After NHS Treatment
Keloids that recur following NHS steroid injections or surgery require comprehensive protocols rarely available through NHS services. These cases benefit from specialist assessment and combination therapies< addressing multiple pathways of keloid formation. Attempting the same failed approach through NHS channels wastes valuable time whilst keloids potentially enlarge.
Ear Keloids Requiring Surgical Revision
Ear keloid surgery requires specific expertise and comprehensive post-operative protocols to prevent the 50-80% recurrence rate seen with basic excision. NHS services may offer simple excision without adequate aftercare, virtually guaranteeing recurrence. Specialist private revision surgery with proper follow-up proves more cost-effective than repeated failed NHS procedures.
Keloids Affecting Quality of Life
When keloids cause significant psychological distress, social anxiety, or functional limitations affecting work or relationships, waiting 12-18 months for limited NHS treatment seems unreasonable. Immediate private intervention can restore quality of life and confidence. The investment in mental wellbeing and social functioning often justifies treatment costs.
Navigating the NHS Referral Process
Understanding how to optimise your NHS referral increases chances of approval and faster access. Strategic approach to the process helps where treatment is genuinely appropriate.
Documenting Symptoms
Keep detailed records of keloid symptoms including pain, itching, restricted movement, or functional impact. Photograph keloids regularly to demonstrate growth progression. This documentation strengthens referral requests and may expedite approval.
GP Communication
Clearly explain functional and psychological impact when requesting referral. GPs have discretion in referral urgency, so effective communication matters. Mention failed over-the-counter treatments and how keloids affect daily life, work, or relationships.
Understanding Rejection Criteria
If CCG rejects funding, request a clear explanation of decision criteria. Some rejections can be appealed with additional supporting information. Understanding specific objections allows you to strengthen subsequent applications or make informed decisions about private treatment.
Combining NHS and Private Treatment
Some patients successfully use hybrid approaches accessing both NHS and private services. Strategic combination can optimise value whilst managing costs.
Initial Assessment Through NHS
Using NHS dermatology consultation for professional diagnosis and assessment provides valuable information even if subsequent treatment occurs privately. This free expert opinion helps you understand your keloid characteristics and treatment needs. You can then make informed decisions about whether private treatment is necessary.
Private Treatment for Complex Cases
Patients might receive basic NHS injections for simple keloids whilst pursuing private treatment for complex or recurrent cases. This targeted private investment addresses cases where NHS services prove inadequate. The approach balances financial considerations with treatment needs.
Switching Between Systems
Starting with NHS treatment then switching to private care if inadequate remains viable. Some patients try NHS options first given the no-cost advantage, moving to private treatment if results disappoint. However, time lost during failed NHS treatment allows keloids to grow, potentially complicating subsequent private treatment.
Conclusion
The NHS does treat keloids, but availability, waiting times, and treatment scope remain significantly limited compared to private services. For symptomatic keloids causing functional problems, NHS treatment may eventually provide adequate care if you can tolerate 12-18 month waits. However, complex cases, recurrent keloids, or situations requiring comprehensive protocols typically necessitate private specialist treatment for optimal outcomes and timely intervention.
Frequently Asked Questions
Does the NHS treat keloids for free?
Yes, NHS keloid treatment is free at point of use for eligible patients, though availability varies substantially by region and clinical need. Treatment typically requires GP referral followed by dermatology or plastic surgery assessment. However, many CCGs restrict NHS keloid treatment to symptomatic cases causing pain or functional impairment, with purely cosmetic concerns often not meeting funding criteria despite significant psychological impact.
How long does it take to get keloid treatment on the NHS?
NHS keloid treatment timelines typically range from 6-18 months from initial GP referral to receiving actual treatment. Initial dermatology consultation waits average 3-6 months, with additional 2-4 months to commence treatment after assessment. Complex cases requiring surgery may face 12-month surgical waiting lists, making total treatment time from decision to completion extend to 2-3 years including follow-up.
What keloid treatments does the NHS offer?
NHS keloid treatment primarily focuses on steroid injections (triamcinolone) as first-line therapy widely available across most regions. Some centres offer cryotherapy, surgical excision, or basic laser treatment, though these remain less accessible. Advanced therapies like combination 5-FU protocols, modern laser systems, or comprehensive surgical revision with proper aftercare are rarely available through NHS services.
Can I get keloid surgery on the NHS?
NHS keloid surgery is possible but generally reserved for large, symptomatic keloids causing significant functional problems. Approval requires demonstrating medical necessity rather than cosmetic concern.
Even when approved, NHS surgical protocols may lack the comprehensive post-operative care essential for preventing 50-80% recurrence rates, potentially making private specialist surgery more cost-effective long-term despite upfront costs.
Why won’t my GP refer me for keloid treatment?
GPs may decline keloid referrals if keloids are considered purely cosmetic without physical symptoms like pain or functional impairment. Local CCG funding criteria often restrict NHS treatment to symptomatic cases.
If your keloid is small, stable, and causing only aesthetic concerns, it may not meet NHS treatment thresholds despite psychological impact being significant to you personally.
Is private keloid treatment better than the NHS?
Private keloid treatment typically offers faster access, advanced technology, and comprehensive protocols combining multiple treatment modalities. NHS services provide proven treatments but with longer waits, basic equipment, and limited session numbers.
For complex or recurrent keloids, private specialist care often produces superior outcomes, whilst simple cases may respond adequately to NHS treatment if patients tolerate waiting periods.
What should I do if NHS treatment fails?
If NHS keloid treatment proves inadequate or keloids recur after NHS intervention, private specialist assessment is warranted. Attempting the same approach repeatedly through NHS channels wastes time whilst keloids potentially enlarge. Private clinics are specifically designed for recurrent or treatment-resistant cases, addressing multiple pathways NHS services cannot access.